Description
Clinical History
A 77-year old male presented with a 3-day history of abdominal and flank pain with fevers and rigors. He was 2 weeks post-operative from a duodenal ulcer repair surgery. He was hypotensive, hyperkalemic and hyponatremic with a purpuric rash. His blood cultures grew Escherichia coli. He failed to respond to treatment, and died soon after admission due to septic shock.
Pathology
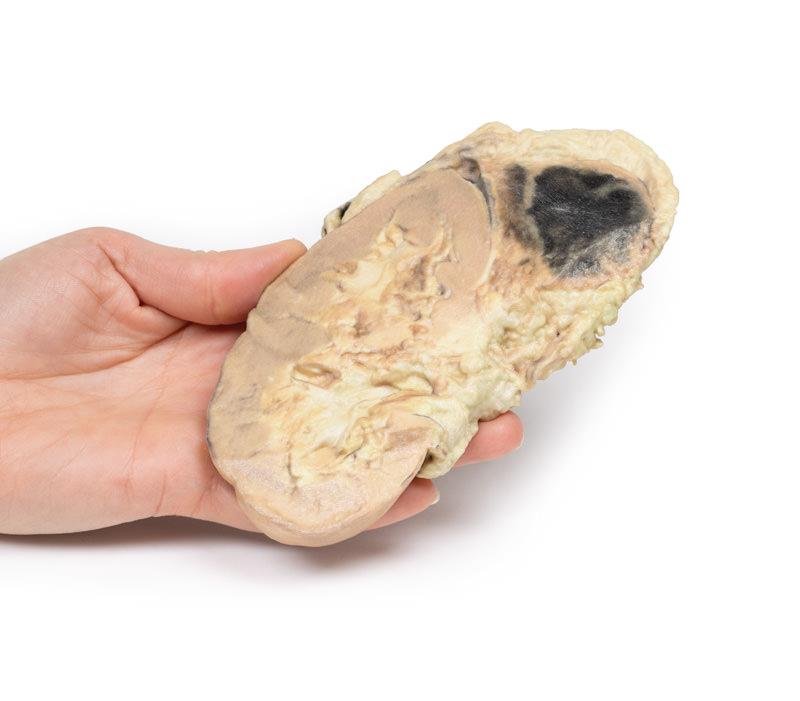
The combined kidney and adrenal gland have been mounted, in order to display the cut surfaces. Extensive haemorrhage has occurred into the adrenal medulla, and there is some extravasation of blood into the periadrenal fat. This is an example of adrenal haemorrhage in the setting of severe septic shock also known as ‘Waterhouse-Friderichsen’ syndrome.
Further Information
Waterhouse-Friderichsen syndrome is characterised by adrenal haemorrhage cause by overwhelming sepsis leading to hypotensive shock, disseminated intravascular coagulation (DIC) and adrenocortical insufficiency. It most commonly occurs in children and rarely in adults. Neisseria meningitis causes over 80% of cases of adrenal haemorrhage. Other organisms that may cause it include Streptococcus pneumoniae, pseudomonas aeruginosa, Escherichia coli, Klebsiella pneumoniae, Haemophilus influenzae and staphylococci.
The exact cause of the haemorrhage is unclear. It may be due to bacterial seeding of the adrenal vessels, to the DIC or to endothelial dysfunction from inflammatory mediators or bacterial toxins. Adrenal haemorrhages can occur bilaterally. The haemorrhage begins in the medulla and extends outwards to the cortex, and may extend into the periadrenal fat. This leads to adrenal gland failure. Patients present with rapidly progressive septic shock, diffuse purpuric skin rash and adrenal insufficiency crisis. Treatment includes supportive therapy, intravenous antibiotics directed against the cultured organisms, and steroid therapy. The mortality rate is over 50%.