Description
Clinical History
A 40-year old male attends his GP complaining of 2 weeks of haematuria and new onset of headache with blurred vision. His GP notes a blood pressure of 260/110 and refers the patient to hospital. The patient collapses on arrival to hospital. A CT brain shows a large subarachnoid haemorrhage from a ruptured ‘berry’ aneurysm. The patient dies shortly after admission.
Pathology
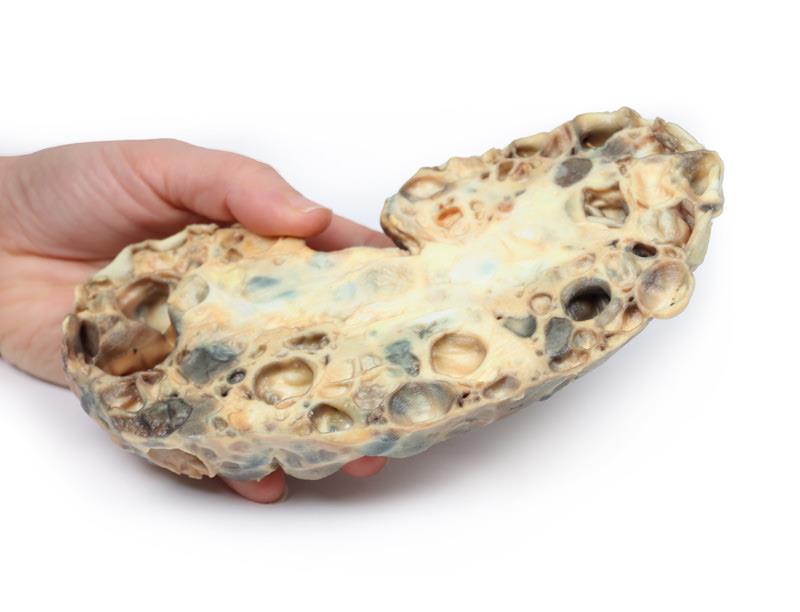
The specimen is an enlarged kidney. The renal parenchyma has been almost completely replaced by numerous dilated cysts varying in size, up to 3cm in diameter. The cysts have thin translucent walls, and some cysts contain material of varying colours, giving a ‘marble-like’ appearance to the cut surface of the kidney. The varying colours are caused by the secretions within the cysts, which may be admixed with haemorrhage. The external surface appears lobulated as a result of multiple projecting cysts. Any remaining renal parenchyma is severely atrophic caused by the pressure of the numerous cysts. This is an example of adult polycystic kidney disease.
Further Information
Adult polycystic kidney disease (APKD) is an autosomal dominant disorder characterised by the presence of multiple cysts within the renal parenchyma. The cysts develop from altered renal tubule epithelium. The cysts expand destroying the glomeruli, causing ischaemia, pressure atrophy, and eventually leading to renal failure.
APKD occurs in 1 in 40 to 1000 live births. Mutations in the PKD1 gene on chromosome 16p13.3 and PKD2 gene on chromosome 4q21 have been described as causal mutations. These code for membrane proteins polycystin 1 and 2, respectively. Patients with PKD1 mutation are more common and have a more severe phenotype. End stage renal disease (ESRD) occurs at a mean age of 74.0 in PKD2 versus 54.3 years in PKD1.
Common symptoms of APKD include haematuria from haemorrhage into cysts and pain or a sensation of dragging from the expansion of cysts and kidney enlargement. Many patients remain asymptomatic until features of renal failure occur such as proteinuria, polyuria, hypertension and uraemia. Extrarenal manifestations of the disease include intracranial ‘berry’ aneurysms, hepatic and pancreatic cysts, as well as mitral valve prolapse and other types of cardiac valve disease. Renal ultrasound is the most common investigation used to diagnose APKD. CT- and MRI scans may also be used as diagnostic tools. Patients with a positive family history of APKD can be offered screening renal US scans and genetic testing in some cases. Treatment involves renal replacement therapy for ESRD and renal transplant (if a donor can be found).
Ultimately, over one-third of patients die from renal failure and one-third from coronary or hypertensive heart disease. Approximately 1% of patients die from subarachnoid haemorrhage, because of berry aneurysm rupture (as in this case). Remaining deaths are due to unrelated causes.