Description
Clinical History
A 60-year-old man head a history of four episodes of severe gripping abdominal pain during the previous year, each lasting two hours and associated with meals. He presented with a similar attack associated with vomiting and fever. This last attack did not resolve spontaneously, and he underwent cholecystectomy.
Pathology
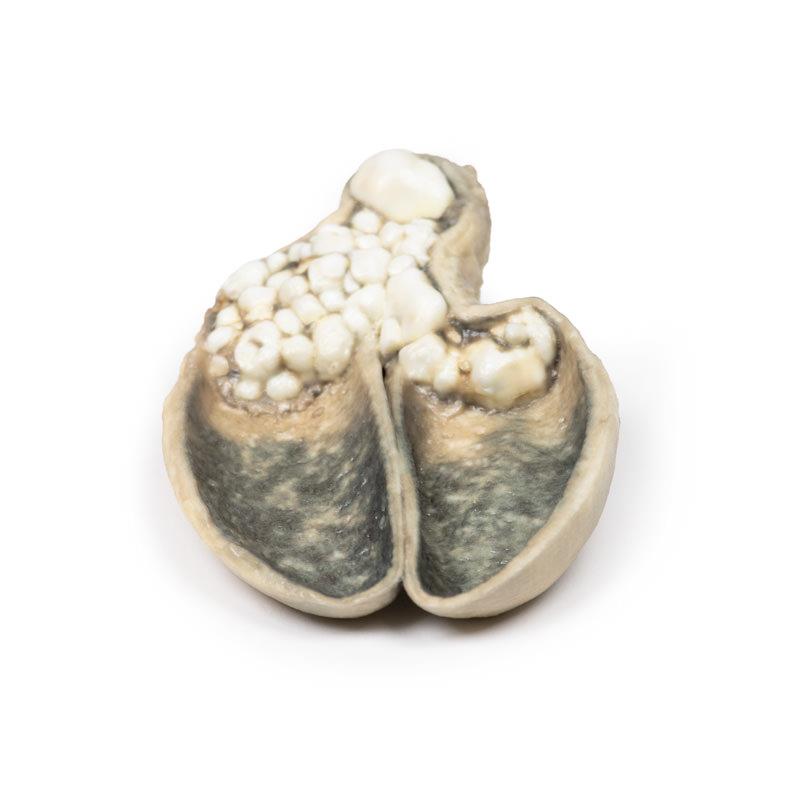
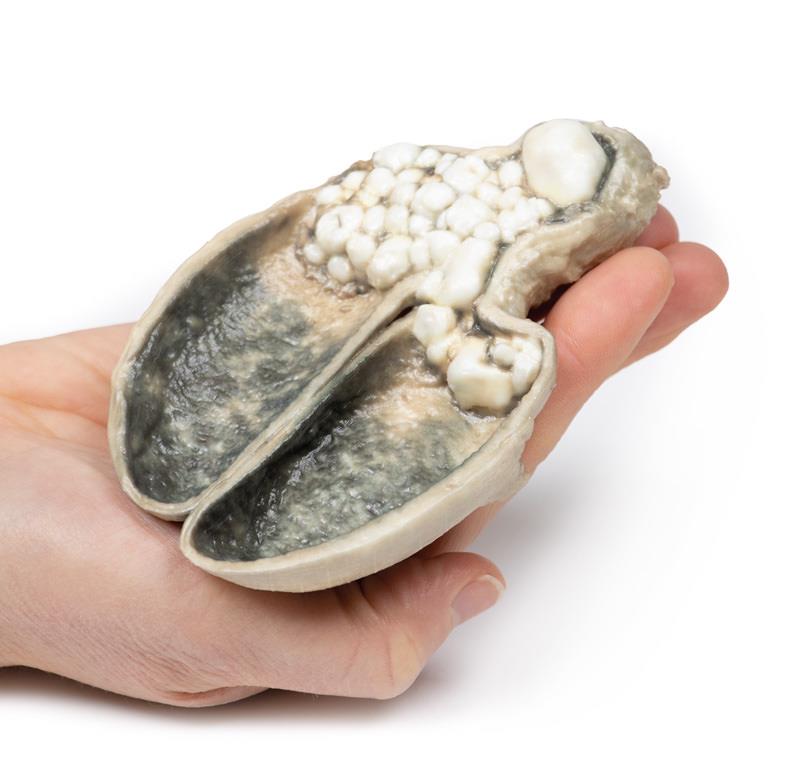
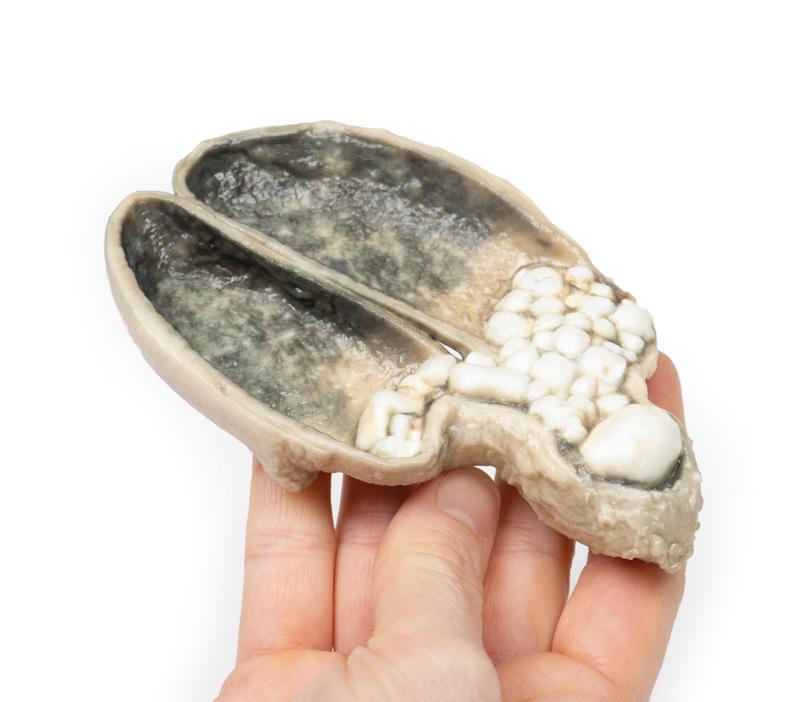
A thick-walled gallbladder has been opened to display a thickened haemorrhagic mucosa and many irregular faceted calculi. A large calculus is impacted in the neck of the gallbladder. The serosal surface of the gall bladder is congested and has lost its normal sheen. This is an example of cholecystitis complicating cholelithiasis (gallstones).
Further Information
Acute cholecystitis is characterised by the clinical syndrome of right upper quadrant pain, fever and jaundice. Gallstones account for the vast majority of acute cholecystitis, with only 5 – 10% of cases being due to other pathology. Chronic cholecystitis may occur, resulting from recurrent attacks and causing fibrosis and thickening of the gallbladder wall. 6-11% of patients with symptomatic gallstones will go on to develop acute cholecystitis. Serum biochemistry will demonstrate leucocytosis with or without obstructive liver function tests. Ultrasound will demonstrate gallstones in the gallbladder, along with wall thickening and a sonographic Murphy’s sign (tenderness from the pressure of the ultrasound probe). Other imaging modalities include nuclear medicine cholescintography scans, MRCP (magnetic cholangiopancreatography) and CT. Endoscopic Retrograde Cholangiopancreatography (ERCP) will provide diagnostic information regarding biliary obstruction and may also be therapeutic. Causative organisms (if present) will be from the gut flora, commonly E coli, Enterococcus, Klebsiella and Enterobacter. Complications include gangrenous cholecystitis, perforation, cholecystoenteric fistula or gallstone ileus. Definitive treatment is surgical cholecystectomy.