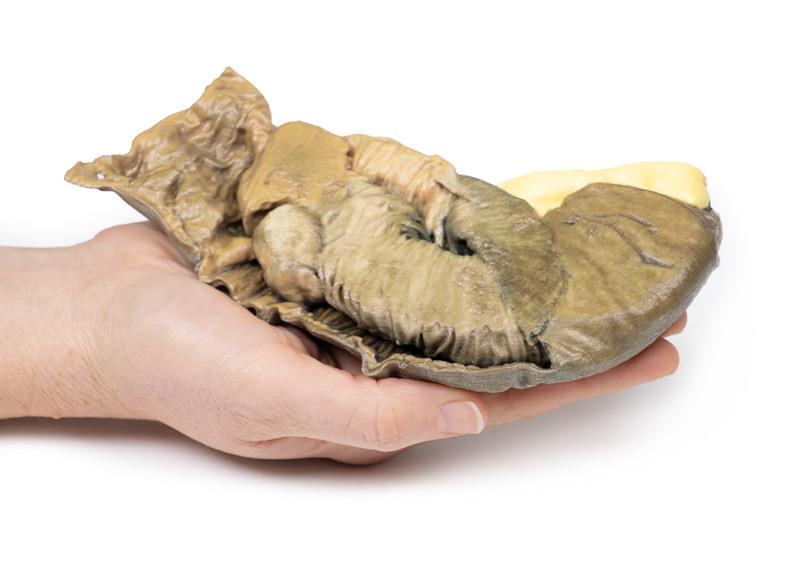
Description
Clinical History
A 66-year-old woman suffered sudden onset of severe colicky central abdominal pain, somewhat relieved by drawing up her knees. She passed a stool containing mucus and blood (“like redcurrant jelly”). On examination, there was a mass in the left hypochondrium, which hardened with each spasm of pain. The specimen was resected at laparotomy.
Pathology
The specimen is a segment of small bowel, approximately 20 cm in length, with attached mesentery up to 2 cm in width (more evident on the uncut aspect of the specimen). About 5 cm from the proximal surgical resection margin (which is at the left hand of the specimen), a polypoid tumour 3 cm in diameter has become invaginated into the lumen of the bowel, and has been propelled distally, forming an intussusception 13 cm in length. The tumour is seen at the apex of the intussusception (near the right hand side of the specimen). The congestion and exudate seen on the mucosal surface of the intussusception (invaginated portion) are features considered with early ischaemic necrosis. The histological diagnosis is not recorded in this case; however, the macroscopic appearance is consistent with a metastatic malignant tumour, although the possibility of a primary tumour cannot definitely be excluded.
Further Information
Intussusception of the small bowel is most common in children, in whom it is usually due to invagination of swollen lymphoid tissue (Peyer‘s patches) in the wall of the distal ileum. In adults, it is rare, causing only between 1 – 5 percent of cases of bowel obstruction. The usual cause a polypoid tumour, as seen in this specimen, acting as a pathological lead point being pulled forward by peristalsis, and thereby causing telescoping of the affected portion of bowel distally. Presentation may be of intermittent symptoms of bowel obstruction and in some cases excruciating pain. Classification of intussusception can be by causal pathology or by location. Abdominal CT scan will typically demonstrate a typical “target sign” with alternating hyper/hypodense layers.