Description
Clinical History
A 64-year old male presents with a 5-month history of generalised malaise, weight loss and dull right flank pain. On examination, there is a palpable right sided abdominal mass. He is noted to be hypertensive. Urinalysis reveals microscopic haematuria. The patient underwent right nephrectomy.
Pathology
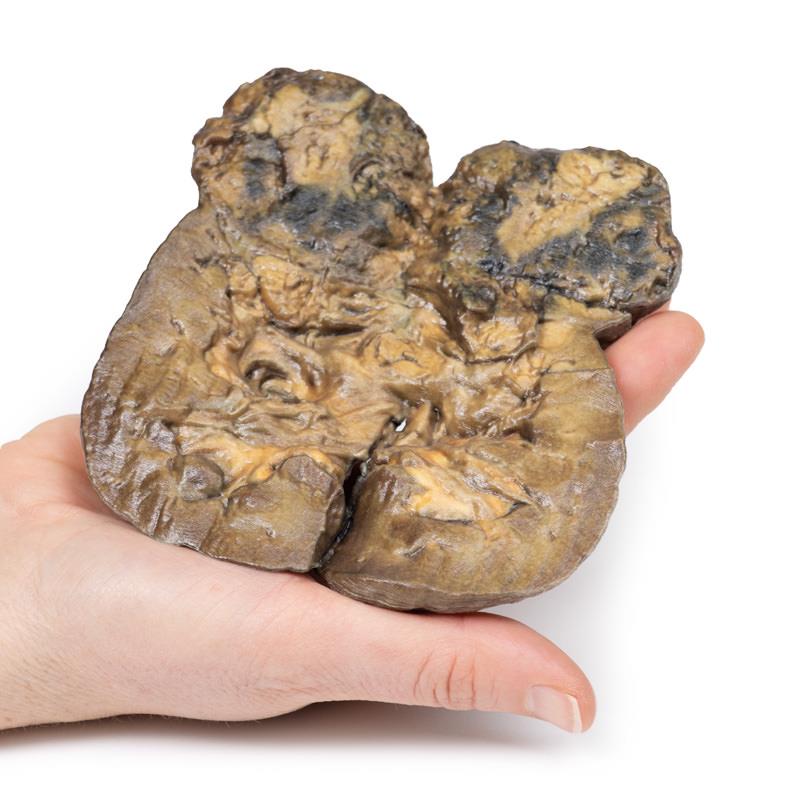
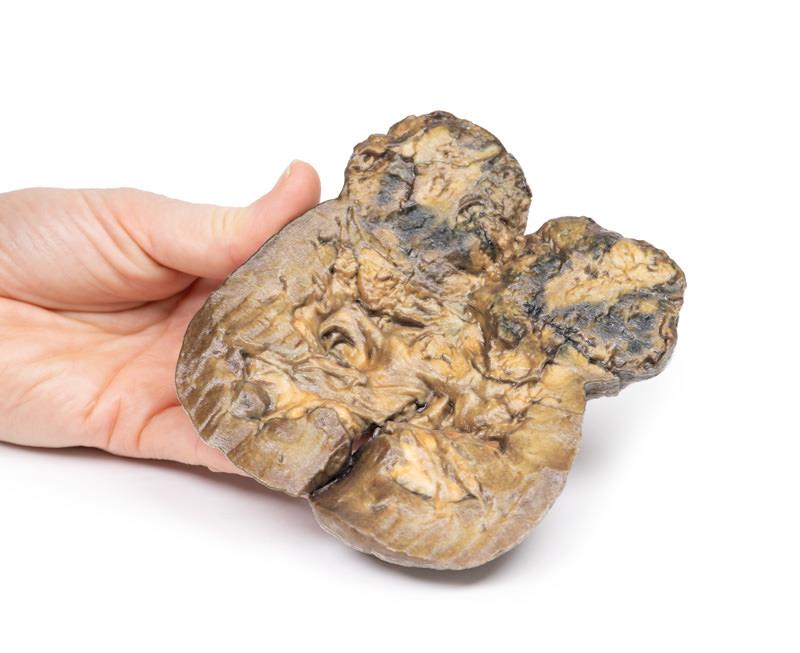
The specimen is a kidney, which has been incompletely dissected in the coronal plane, and mounted to display the cut surface. The lower pole of the kidney has been replaced by a rounded ill-defined irregular mass 5cm in diameter, which has compressed and distorted the overlying renal parenchyma. The cut surface of the tumour has a variegated appearance caused by areas of haemorrhage and necrosis. Several small pale-yellow tumour nodules are present in the cortex and medulla above and separate from the lower pole tumour. These are intrarenal metastases. The renal pelvis appears slightly dilated with some blunting of the renal papillae, suggesting a degree of hydronephrosis. The capsular surface is finely nodular with a few coarse scars and contains several small simple cysts (see rear of specimen). Histologically, the tumour was diagnosed as a renal cell carcinoma.
Further Information
Renal cell carcinoma (RCC) comprise 85% of the primary renal malignancies. They originate within the renal cortex. The risk of developing RCC is doubled in males. It most commonly occurs in the 6th decade of life. Other risk factors for RCC include smoking, obesity, hypertension, unopposed estrogen therapy, as well as exposure to asbestos, petroleum and heavy metals. Most RCC are sporadic but around 5% are due to autosomal dominant familial cancers, such as Von Hippel Lindau syndrome, hereditary leiomyomatosis and Birt-Hogg-Dubé syndrome.
There are several major primary renal tumour types according to genetic and histological tumour characteristics: clear cell carcinoma (70-80%), papillary carcinoma (10-15%), chromophobe carcinoma (5-10%), oncytic carcinoma (3-7%) and collecting (Bellini) Duct carcinoma (<1%).
Clear cell carcinoma typically have a deletion of chromosome 3p and arise from the proximal tubule. They may be solid or less commonly cystic. They occur in association with Von Hippel Lindau as well as sporadically. Papillary carcinomas arise from the proximal tubule. They are associated with trisomies 7 and 17; loss of Y in male patients; and MET kinase domain mutations. They are frequently multifocal in origin. Chromophobe carcinoma originate from intercalated cells of the collecting ducts. They are associated with multiple chromosome losses and hypodiploidy. They have a low risk of disease progression.
Renal oncocytic carcinomas are typically comprised of well-differentiated cells with prominently eosinophilic granular cytoplasm; they are associated with a good prognosis. In contrast, collecting (Bellini) duct carcinoma of the kidney is a highly aggressive tumour with an extremely poor prognosis as it does not respond well to chemotherapy drugs used for renal cell carcinoma, and progresses and spreads more quickly. It is a variety of renal cell carcinoma (RCC) arising from the distal segment of the collecting ducts of Bellini in the renal medulla.
The typical clinical features of RCC are costovertebral pain, palpable mass and haematuria. RCC is the great mimic in medicine producing many manifestations including: polycythemia, hypercalcaemia, hypertension, pyrexia, Cushing‘s syndrome, eosinophilia and amyloidosis. RCC tend to metastasize before producing may local symptoms. The most common sites of distal spread are the lungs (50%) and bones (33%) followed by lymph nodes, adrenal glands and brain. RCC has a tendency to invade
the renal vein and extend up it as a tumour thrombus, growing as a solid column extending upto the inferior vena cava.
Ultrasound and CT are the most common investigations used to assess renal lesions and diagnose RCC. A tissue biopsy may be required in some patients. An increasing number of patients are being diagnosed with RCC because of incidental kidney lesions being detected on abdominal CT requested for other medical reasons.
The average 5-year survival rate for RCC is 70%. Treatment depends on the stage of the tumour. Radical nephrectomy is the usual surgical option. Medical treatment includes chemotherapeutic drugs as well as Vascular endothelial growth factor (VEGF) inhibitors and tyrosine kinases inhibitors in patients with metastatic disease.