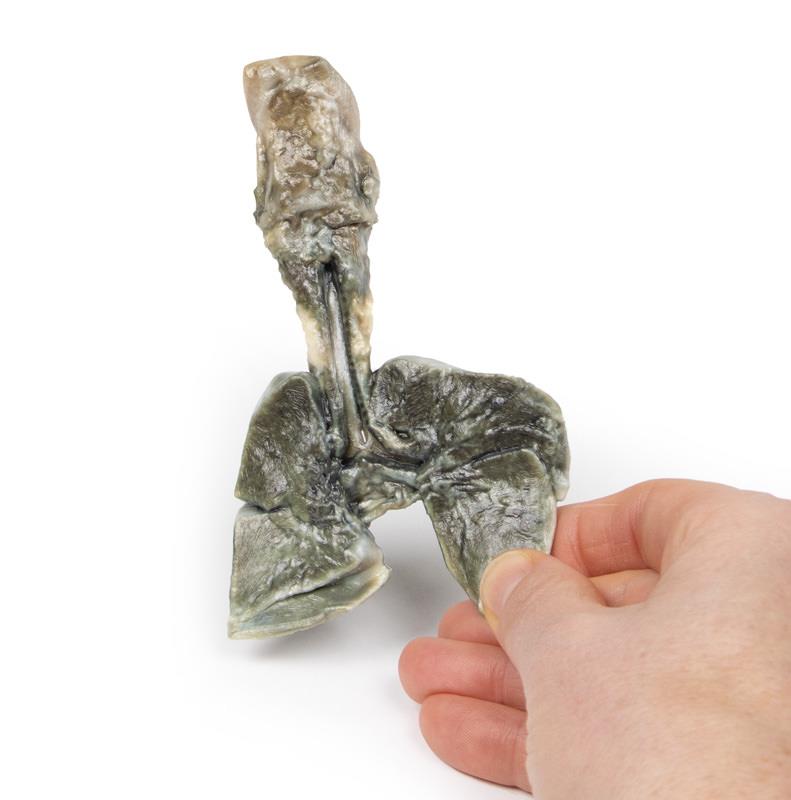
Description
Clinical History
A 32-year-old female G3P0 (gravida 3, para 0‘ – i.e., has had two pregnancies, with neither of the embyros surviving to a gestational age of 24 weeks) presents in preterm labour at 25 weeks gestation. The GP had noted an increased fundal height at 30cm one week prior, but the mother had refused prenatal testing or ultrasound, and was lost to follow up. She delivered a live born male baby. Examination of the baby noted polydactyly, imperforate anus, excessive drooling, and a loud pan-systolic murmur. A single umbilical artery was noted in the umbilical cord. The baby had difficulty feeding with increasing respiratory distress. The baby died 2 days later from aspiration pneumonia.
Pathology/Specimen Details
The specimen comprises the tongue, larynx, trachea, bronchi, both lungs and oesophagus of the foetus. The trachea and bronchi have been divided in the midline. A fistula is present just above the bifurcation at a communicating fistula can be seen connecting the distal oesophagus to the trachea (arrow). This is an example of a Type C Tracheoesophageal Fistula (oesophageal atresia with distal tracheoesophageal fistula). It is difficult to discern if the oesophagus ends as a blind pouch at the lower extent of the specimen.
Further Information
Tracheoesophageal Fistula (TEF) is a common congenital abnormality occurring in about 1 in 4000 live births. TEF usually occurs with oesophageal atresia (sometimes abbreviated to EA, reflecting the US spelling of ‘esophagus’). TEF are classified according to their anatomical configuration. Type C is the most common configuration; as described above, in which oesophageal atresia with distal tracheoesophageal fistula making up 86% of cases. TEF occurs without oesophageal atresia in only 4% of cases, Type E.
TEF and oesophageal atresia are caused by defective lateral septation of the foregut into the oesophagus and trachea. It is believed that a defect in epithelial-mesenchymal interactions causes failed branching of a lung bud branch which becomes the fistula tract. It is associated with VACTERL (vertebral defects, anal atresia, cardiac defects, TEF, renal anomalies, and limb abnormalities) or CHARGE syndrome (Coloboma, Heart defects, Atresia choanae, Growth retardation, Genital abnormalities, and Ear abnormalities).
Oesophageal atresia can be seen on prenatal ultrasound as polyhydramnios, absent/collapsed stomach, and proximal oesophageal pouch dilation. EA with TEF can be more difficult to see on ultrasound as fistula allows fluid flow into the stomach. Polyhydramnios occurs in one third of cases of EA with distal TEF. Postnatal symptoms vary on the configuration of the fistula. These include excessive drooling, respiratory distress, difficulty feeding and choking. Reflux of gastric contents can lead to aspiration pneumonia as in this case.
Diagnosis can be made by failing to pass a nasogastric tube into the stomach along with X-ray imaging. Fluoroscopy with contrast can be used for more indeterminate cases. For milder cases diagnosis may be made later with endoscopic investigation. Treatment involves surgical correction of the defects. Prognosis is usually good. However, cases with associated chromosomal, prematurity and cardiac defects are at increased risk of death.