Description
Clinical History
A 36-year old female was admitted to hospital with a 3-week history of bloody diarrhoea and lower abdominal pain. Further history taking revealed 4 similar episodes of diarrhoea and abdominal pain of over the past 7 years. Sigmoidoscopy showed a erythematous, ulcerated and oedematous rectal mucosa. She was commenced on steroid treatment but her symptoms failed to improve. She underwent a total colectomy.
Pathology
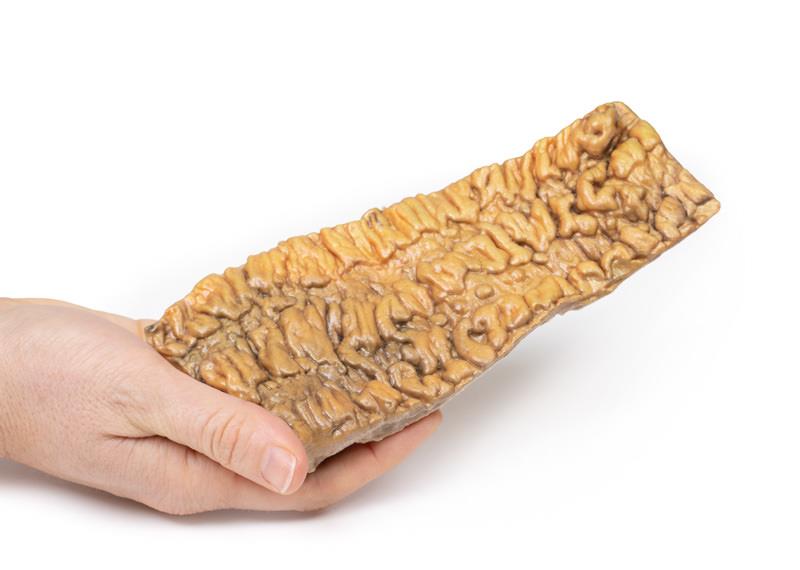
The resected colon has been sliced open longitudinally to show the mucosal surface. There is extensive confluent ulceration separated by oedematous islands of residual mucosa. The ulcers have necrotic bases with overhanging edges some of which form ‘pseudo’-polyps. Histology of the bowel mucosa showed acute inflammatory changes with crypt abscesses, focal necrosis and ulceration. This is an example of acute ulcerative colitis (UC).
Further Information
Ulcerative colitis is a chronic ulcero-inflammatory disease that usually involves the rectum and can extend proximally in a continuous pattern to involve other parts to the colon. The inflammatory process is diffuse but is generally limited to the mucosa and superficial submucosa. The triggering factor for UC in unknown. It most commonly begins between the ages of 15-25 years and is slightly more common in females.
UC patients can present with diarrhoea, which may contain blood or mucus, faecal urgency, faecal frequency, tenesmus, colicky abdominal pain, as well as weight loss, anaemia and fatigue. Colonic inflammation can lead to toxic megacolon, colonic perforation or colon cancer. Extraintestinal manifestations include anterior uveitis, migrating polyarthritis, sacroileitis, ankylosing spondylitis, erythema nodosum, pyoderma gangrenosum and primary sclerosing cholangitis.
Treatments of UC include use of anti-inflammatory drugs such as steroids, disease modifying rheumatoid drug and TNF (tumor necrosis factor) inhibitors. Colectomy essentially cures intestinal symptoms of UC but extraintestinal manifestations of the disease may persist.